This was published 7 months ago
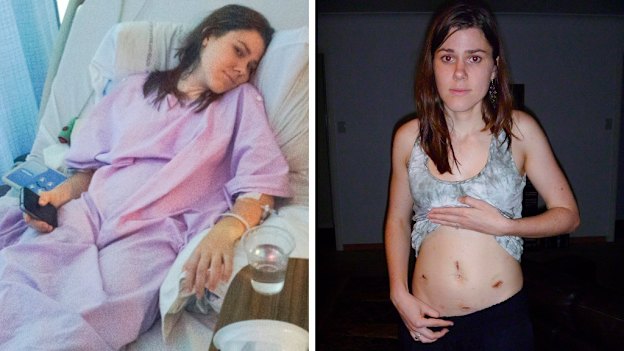
Fatima was left for hours in extreme pain awaiting treatment. She almost lost her ovary

It was life’s cruellest lottery and Fatima Azhar wasn’t prepared to roll the dice.
The 37-year-old and her husband had already been dealt a luckless hand. They discovered they both carried the same rare genetic condition – spinal muscular atrophy – which causes progressive muscle wastage and is the leading genetic cause of infant death.
Should the couple try to conceive naturally, they faced a one in four chance of passing the disease to their offspring. They didn’t need the gravity of their situation explained: the disease had already afflicted two young members of their extended family.
IVF promised to all but erase those risks, smoothing their path to a healthy baby. Without hesitation, the Melbourne couple embarked on their first cycle.
But Azhar says she was never warned about the dangers the treatments posed to her own health. She was blindsided when a cascade of troubling events nearly resulted in the death of one of her ovaries.
Like more than 2000 women who have responded to the Herald and The Age’s survey as part of our series on medical misogyny, Azhar recalls her initial concerns were dismissed, which led to treatment delays and agonising pain during what would prove a time-critical medical emergency.
“I was left in extreme pain for hours, with no clear updates on what was happening or what the next steps would be,” Azhar said of her presentation to a hospital emergency department, three weeks after her egg retrieval in 2020. “I repeatedly called out to the nurses and doctors, but there was little response.”
Azhar was suffering from ovarian torsion, a gynaecological emergency affecting about 9.9 out of every 100,000 women of reproductive age.
It occurs when the ovary twists on its ligaments, severing its own blood supply. A narrow window of time exists to operate and save the organ before it becomes necrotic and dies.
‘I repeatedly called out to the nurses and doctors, but there was little response.’Fatima Azhar
Leading emergency doctors, gynaecologists and lawyers say failings in Australia’s health system are causing avoidable delays in the diagnosis and treatment of ovarian torsion, with sometimes catastrophic results for the women involved.
They include the loss of the ovary and fallopian tube, potentially affecting fertility. Other complications include infections such as peritonitis and sepsis, adhesions and chronic pain.
Experts flagged a lack of pelvic ultrasound availability and gynaecological services at many emergency departments across the country as the most pressing shortcoming contributing to delayed diagnoses.
Dr Sarah Whitelaw, an emergency doctor and an Australian Medical Association federal council member, said patients were being “set up to fail” if their outcomes depended on which hospital they chose to attend.

“While we’ve got system issues like that, we’re going to continue to have women lose their ovaries unnecessarily,” she said.
The experts are speaking out as a series by the Herald and the Age shines a light on medical misogyny. The investigation is not seeking to lay blame at the feet of clinicians but rather to expose the entrenched, structural problems disadvantaging women in a health system that historically evolved to reflect the needs of men.
It’s a term also adopted by the federal government, which has cited mounting Australian and international research showing women disproportionately experience diagnosis and treatment delays, and an underestimation of their pain.
Lights and sirens
In 2020, a study in the US, ‘The Twisted Truth’, revealed troubling differences in the handling of ovarian torsion when compared to testicular torsion, a condition in males in which the testicle twists and cuts off its blood supply.
The team from Louisiana State University’s School of Medicine measured “decision-to-incision” time – the lag between the decision to operate and the beginning of emergency surgery – over four years at a large tertiary referral centre.
The mean “decision-to-incision” time for ovarian torsion was 153 minutes: almost double the 80 minutes for testicular torsion.
The findings reverberated internationally, including in Australia, where some local doctors harboured concerns that suspected testicular torsion cases were being treated with greater urgency than suspected ovarian torsion.
It’s something that concerns Dr Jillann Farmer, a former UN medical director, due to what she has witnessed in her line of work as an emergency GP in rural Queensland.
A suspected testicular torsion case “went up the road with lights and sirens straight to theatre”, while it was suggested a “wait-and-see” approach would be appropriate for the woman with suspected ovarian torsion.
“That contrast really struck me,” she said. “With a little bit of advocacy, she did go to theatre, and the ovary was saved.”
Farmer is calling for the establishment of a national registry with data on time to presentation and time to theatre for ovarian torsion cases.
“If you’re not measuring it, your eyes won’t see it,” she said.
However, Farmer was also among several doctors who said the diagnosis of testicular and ovarian torsion was far from an “apples to apples” comparison.
The former is much simpler to diagnose because the testes are easier to examine as they are outside the body and the pain is localised.
The dilemma facing doctors is that ovarian torsion tends to cause vague abdominal pain, meaning there could be myriad explanations, including appendicitis, ectopic pregnancy or a ruptured cyst. Often, a diagnosis can be made only at surgery.
However, experts interviewed by this masthead were in broad agreement that resourcing issues in emergency departments were often a significant roadblock to the swift diagnosis of ovarian torsion.
A gynaecologist is best placed to diagnose and treat ovarian torsion, and usually relies on the findings of a pelvic ultrasound, which they either perform themselves or it is outsourced to a sonographer.

These are not the kind of resources always readily available when a patient presents to the emergency department.
Royal Australian and New Zealand College of Obstetricians and Gynaecologists president-elect Dr Nisha Khot said a pelvic ultrasound was a very specialised scan.
“It’s not a scan that sits in the skillset of people who would be working in a general emergency department,” she said.
Khot said there were particular difficulties in accessing such scans after hours and in regional and remote locations. The problem was further compounded by a nationwide shortage of sonographers.
National malady
The problems may be most pronounced in the bush but capital cities are far from immune.
More than a decade after the death of her ovary and fallopian tube, Brisbane woman Irena Black is still haunted by the possibility of a different outcome had she gone under the knife on the day she had presented to the emergency department.

In 2013, the then 22-year-old attended the Prince Charles Hospital, a major teaching hospital in the Brisbane suburb of Chermside, with severe abdominal pain.
“I didn’t know when I went there they didn’t have a gynaecological unit,” she recalled.
Black was asked to rate her pain, telling staff it was a seven out of 10.
“They told me that couldn’t be right. ‘If it was that bad you wouldn’t be able to walk’. And I was like, ‘oh, I don’t know then, a five?’,” Black said.
The hospital ran a battery of tests, but Black said she was told she would be sent home if an ultrasound didn’t detect anything. The tenor of the conversations quickly changed when the ultrasound revealed a large mass on her ovary.
It was decided she needed to be transferred to the Royal Brisbane and Women’s Hospital, where another five agonising hours elapsed.
“When I got there because it was dark – all the surgeons had gone home,” she said.
Black’s surgery was scheduled for the following afternoon.
“When they got in there, both the ovary and tube were necrotic because they’d been dead for so long,” she said.
Black bled so profusely she required two blood transfusions.
“I didn’t know why I waited so long,” she said. “I assume there were more priority surgeries.”
Both hospitals fall under the jurisdiction of Metro North Health. A spokesman said its hospitals were committed to the timely diagnosis and escalation of time-critical conditions.
“While we are unable to comment on specific patient cases, Metro North Health has rigorous procedures in relation to care of time sensitive conditions,” he said.
He said transfer of patients to a specialist unit at another hospital was required at times to ensure the most appropriate care was provided.
“Metro North Health practices in line with clinical guidelines for ovarian torsion, which outline diagnosis, imaging, and management of the condition.”
Delayed and dismissed
Hayley Collins, a special counsel in the NSW Hunter region, has acted for patients in multiple medical negligence cases involving ovarian torsion.
Usually those patients had presented at least once to hospital and had been discharged without a diagnosis, said Collins, from the Law Office of Conrad Curry in Newcastle.
In one case, the patient had been sent away three times.
“Unfortunately one of the themes we see is the health professional assuming something else is responsible for a client’s symptoms and not acting with the urgency that it requires,” Collins said.
Improving ultrasound facilities at hospitals could curb the need for patients to be sent away for outpatient scans, she said.
Upon leaving the hospital, things could go awry for the patient, particularly if the ultrasound clinic hadn’t been given clear guidance about the suspicions of ovarian torsion or plans for the communication of results.

“All of that can lead to diagnosis being delayed,” Collins said.
A sonographer, who requested anonymity to speak freely, said it was vital they were made aware of suspicions of ovarian torsion so patients could be seen urgently – otherwise they could wait up to a week for an appointment, and the opportunity to save the ovary could be lost.
Postcode lottery
Very complex diagnoses such as ovarian torsion were more likely to be missed in overburdened emergency departments, Whitelaw said.
“If your system rewards seeing people very quickly, we’re going to get it wrong in critical conditions like ovarian torsion,” Whitelaw said.
Farmer was concerned junior doctors in resource-stretched environments were sometimes hesitant to mobilise on-call staff if there was a lot of uncertainty surrounding the diagnosis.
Calling in a sonographer after hours could mean such services weren’t available the following day.
“There can be a sense we shouldn’t be waking people in the night when it could be a cyst, or endometriosis,” Farmer said.
Farmer said staff in such scenarios would benefit from clearer guidelines on when to contact on-call staff.
Whitelaw also said a pelvic ultrasound is rebated at a lower rate than a testicular ultrasound, even though the former is more time-consuming and complex.
“There is no one sitting there saying ‘we want to deny people an ultrasound’, but it’s something that’s not given the priority that it needs and deserves,” she said.
Dr Stephen Lee has witnessed firsthand the real-world impact of prioritising those services at Australia’s oldest specialist women’s hospital.
Some years ago, Melbourne’s Royal Women’s Hospital flagged the delayed management of ovarian torsion as an area for improvement.
Lee, who leads the hospital’s acute gynaecology unit, said a joint meeting of the ultrasound and gynaecology departments was convened to address the issue.

The team developed a protocol to prioritise an early review by a gynaecologist and immediate diagnostic ultrasound where torsion was suspected, regardless of the time of day.
Lee said they had observed significantly fewer cases of delayed management since.
“In my view, the management of ovarian torsion at the Royal Women’s Hospital is world-class,” he said.
Lee said that while gynaecological ultrasound remained the best diagnostic tool available, it had an accuracy rate of only about 70 per cent.
MEDICAL MISOGYNY: A CALL TO ACTION
The Sydney Morning Herald and The Age last year launched an investigation into medical misogyny: ingrained, systemic sexism across Australia’s healthcare system, medical research and practise.
More than 2000 women shared their experiences as part of our crowd-sourced investigative series, which prompted a national outpouring of grief and frustration as women described feeling gaslit, dismissed or being told their pain was “all in their heads”.
We call on the federal government to boost Medicare funding for GP appointments that last more than 20 minutes to improve care for women and others with complex health conditions.
The Albanese government and the Coalition have promised to pour $8.5 billion into Medicare to make GP visits more affordable and improve bulk billing rates, but longer 20-minute appointments will receive a smaller proportional funding increase.
Doctors have warned that these policies could further disadvantage women by continuing to incentivise shorter consultations, which don’t give GPs enough time to address menopause, pelvic pain and other women’s health issues.
“The development of more precise diagnostic tools would be a significant step forward for the hundreds of Victorian women who experience ovarian torsion each year,” he said.
Like Farmer and Khot, Lee drew attention to the paucity of data measuring the performance of emergency departments in managing ovarian torsion.
He suspected there would be higher incidences of delays in those that lacked gynaecological ultrasound services, but said better data collection was needed to test that hypothesis.
But to Dr Rachael Gill, acting NSW faculty chair of the Australasian College for Emergency Medicine, the need for improved funding to bridge the postcode divide was already clear.
“We need more investment in publicly funded diagnostic imaging services, as well as inpatient and outpatient gynaecological clinics, in all areas,” she said.
‘I couldn’t stand upright’
The red flag was only subtle but Fatima Azhar had an uneasy sense something wasn’t right. She was troubled by a dull throbbing pain in her back and left side, about a week after her first IVF retrieval in July 2020.
Azhar’s high yield of 33 eggs was a double-edged sword: it bolstered her chances of a live birth, but also of complications such as ovarian torsion. However, she says her IVF clinic never informed her of the heightened risk.
When Azhar queried the back pain with the nursing staff, she was told it was probably due to the number of eggs collected and to consult a GP if she was concerned. “No follow-up scan or check was arranged,” she said.
A couple of days later, Azhar keeled over as the pain rapidly intensified.
“It was so intense I couldn’t stand upright,” Azhar said.
She rushed to the emergency department at Dandenong Hospital in Melbourne’s south-east, arriving just before 6pm.
The hospital has an obstetrics and gynaecology registrar available on site 24 hours a day.
However, Azhar says she was left unattended for about four hours before she was wheeled away for a pelvic ultrasound.
“Despite being in significant pain and unable to stand upright, it took hours before any real action was taken,” she said.
“The area I was taken to for the scan was quite empty and felt very deserted. That may have contributed to the delay.”
The ultrasound revealed her left ovary had swelled to seven centimetres (the average size is four centimetres) and blood flow to it had been reduced significantly. The treating team strongly suspected ovarian torsion.
‘It was the most painful five hours of my life.’Fatima Azhar
“I was then left alone on a bed outside the scan room for about another hour,” she said. “Even morphine didn’t ease the pain. Instead, it added nausea to the experience.”
Emergency surgery revealed a 720-degree torsion of the ovary and fallopian tube. Azhar’s ovary was saved, but the experience left her traumatised.
“It was the most painful five hours of my life,” she said.
A Monash Health spokeswoman said it did not provide details about patients or their care due to confidentiality requirements. However, she said wait times at emergency departments varied, as patients were seen in order of clinical urgency.
“The most sick or injured are always cared for first,” the spokeswoman said. “Our hospitals want to treat every patient as soon as possible. We understand and empathise that waiting for care can be stressful.”
Azhar wrote a letter expressing her concerns to her IVF clinic, which she has requested not be named as she is still undergoing treatments.
She questioned why there hadn’t been closer monitoring or a more proactive response when she first reported her pain.
“After my complaint, two follow-up scans were arranged, spaced a few days apart, to check for reduction in ovary size – something I believe should have happened from the outset,” she said.
None of Azhar’s four healthy embryos from that cycle successfully implanted. She underwent another egg retrieval, and this time she was given a brochure outlining potential complications.
Azhar is calling for IVF clinics to improve monitoring of patients who retrieve large numbers of eggs and communication about potential complications before patients undergo treatment.
“So they know what’s normal, what’s not and when to seek help,” she said.
Azhar also wants to see greater awareness in emergency departments about IVF-related complications such as ovarian torsion.
The Fertility Society of Australia and New Zealand is the peak body representing fertility doctors, nurses and scientists.
A spokeswoman said that under the Reproductive Technology Accreditation Committee’s code of practice, clinics must provide written and verbal information about the risks of treatments, including complications, in a format and language appropriate to the patient.
“This is also embedded in the consent process and patient education protocols and is subject to regular review through internal and external audits by RTAC and third-party auditors,” she said.
The spokeswoman said clinics also had to ensure patients received information on how to access care after hours or in an emergency. They are explicitly required to identify and manage patients at risk of complications, such as ovarian hyperstimulation syndrome and ovarian torsion.
“High egg yields are a known risk factor for OHSS and, indirectly, ovarian torsion,” she said.
“The code requires proactive monitoring (e.g. follow-up calls, symptom checks) to detect and respond to risks early, and to report any hospitalisation or serious complication to RTAC.”
If ovarian torsion occurs within four weeks of retrieval and requires a hospital admission exceeding 24 hours, it is defined as a serious adverse event. The clinic must report it, follow up with the patient and review the case to identify if any corrective actions are needed.
“Diagnosis and emergency management of ovarian torsion are hospital or specialist duties, but it is still the IVF clinic’s responsibility for surveillance, timely referral, and adverse-event reporting,” the spokeswoman said.
Start the day with a summary of the day’s most important and interesting stories, analysis and insights. Sign up for our Morning Edition newsletter.